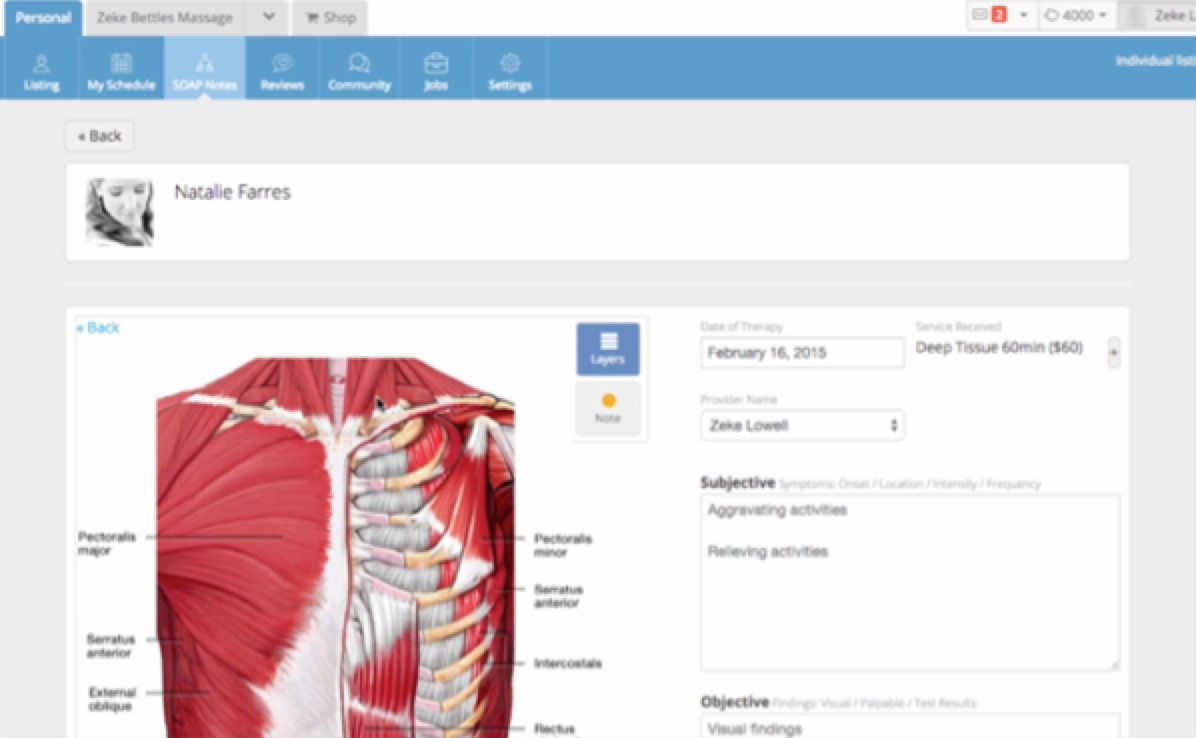
SOAP Notes—Subjective, Objective, Assessment, and Plan—allow wellness practitioners to document and organize client progress for themselves and communicate patient issues clearly to other healthcare professionals. They may also be required for insurance billing. As any bodyworker or massage therapist knows, documentation can require a lot of time and effort (especially if your day is packed and you’re running behind), but they’re also essential to providing customized service to your returning clientele and integrating your bodywork services into a client’s overall healthcare team.
SOAP notes are easy to use and seamlessly connected to a client’s appointment records. Document the troubling areas for your client; take notes of any medications that they may be on; their last visit, and any new, additional issues that arise. Track your clients’ progress with detailed SOAP notes that allow you to take your practice to the next level by staying organized, building confidence, and facilitating long-term relationships with loyal clientele.
Here are three tips for keeping your SOAP notes simplified:
1. Ask your clients the right questions
Clients are naturally drawn to one part of the body to pinpoint, but it’s important that a massage therapist gets the whole picture of health. Therefore, try asking open-ended questions to clients and then directing them a bit further.
“Where should our focus be today?” is always a great place to start. This allows the client to tell you where on their body is causing the most pain or trouble.
“Are you seeing any other physicians, and if so, for what?” will also give you a great idea of how the rest of the client’s health is—and maybe some areas or techniques to avoid for maximum comfort.
“What do you find aggravates your condition?” is also key to ask clients. Sometimes they may not be sure, and you can help them think about their daily activities that may need reworking. Make notes on the client’s emotional and physical status, but only their direct remarks about each.
2. Don’t rely on your memory
Don’t wait until after an appointment or even after your workday to begin making notes! If you’re too busy to take proper notes between sessions, consider taking short notes to expand on later when you have more time.
Take notes as the client talks on a computer or tablet without the hassle of writing them down and transferring them later. This is essential so that you don’t forget any helpful or important information.
Take notes on both the subjective remarks (“It’s hard for me to pick up my child”) and objective observations (“Client is limping on left side”).
3. Brevity is best
When it comes to SOAP notes, brevity is best. You want to be sure you have a thorough account of the client’s activities, areas of trouble, and services rendered, but you do not want to have a lengthy novel on your hands each time a client visits. This is important not only for your time and efficiency but also for your recall and insurance purposes.
If you’re looking for seamlessly integrated SOAP notes that almost write themselves, try our premium SOAP notes free for 30 days.
Not quite ready to join MassageBook? With our free massage therapy SOAP note form, you can still experience the benefits of digital SOAP notes today.
- Author: Mark Volkmann
- Published: May 20, 2015
Grow and simplify your practice!
Related Posts
Top Massage Resources
Categories
Categories Index ( 21 )
- Friday focus (9)
- Massage therapists (42)
- Massage therapy benefits (7)
- Marketing (160)
- Massagebook features (12)
- Healthy living (12)
- Press (2)
- Practice management (56)
- From our ceo (3)
- Software releases (23)
- Education (5)
- People focus (3)
- Types of therapy (1)
- Uncategorized (1)
- Massagebook (36)
- Massage therapy (4)
- Massage practice (1)
- Massagebook (1)
- Fun (1)
- Guest blog (1)
- Resources (2)